Adams Kirurgia Kliinik
Bariatric, postbariatric and general surgery
Laparoscopic cholecystectomy
Cholelithiasis is a very common upper gastrointestinal tract disease, which has many forms from asymptomatic gallstones to acute gangrenous-perforated cholecystitis. The abovementioned disease occurs in up to 11 % of male and up to 26% of female population. In case of 10-20% of the patients cholelithiasis is expressed as strong upper abdominal pain episodes occurring at various frequencies. The pain may radiate to the right scapula or shoulder joint area or above the clavicle. Usually a “heavy and plentiful” meal preceding a pain episode can be identified as a provocative factor. Dull gnawing pain of chronic nature localizing under the right costal pleura, abdominal tension and occasional nausea may occur. In such a case surgical treatment is indicated for prevention of complications.
Gallstones are hard deposits in the gallbladder, which can differ greatly in size, consistency and colour (with a diameter of 1-2 mm up to 5-7 cm) at the moment they are detected. They form as a result of changes in bile composition, which, in turn, may have very different causes. The need for surgery does not depend on the amount or size of the stones, but primarily on the existence of complaints. Gigantic > 3 cm stones, in the existence of which it is highly likely that complications occur and surgery is indicated in any case, are an exception. If gallstones are found (ultrasonography is the most certain method), you should see a surgeon within 1 month for drawing up the further treatment plan.
The complications of cholelithiasis include acute cholecystitis, cholangitis, icterus caused by mechanical biliary obstruction (a stone blocks bile flow) and pancreatitis. Mortality in case of pancreatitis alone is 10%. These medical conditions require emergency medical intervention.
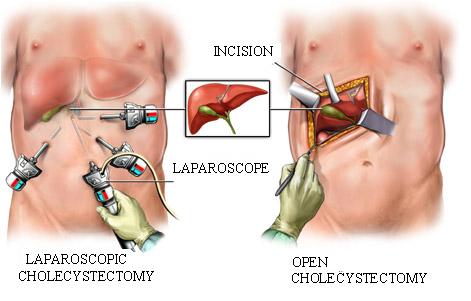
Cholelithiasis requires surgical treatment. A distinction is made between closed, i.e. laparoscopic and conventional, i.e. open method.
The laparoscopic method is preferred (successful in 96 – 98% of cases, i.e. there is no need to switch to the open method during operation), but sometimes it can be technically very complicated and then the so-called “open method” should be used, i.e. a longer skin incision is made. Laparoscopic cholecystectomy i.e. gallbladder removal is carried out under general anesthesia (the patient is sleeping). Instruments are inserted into the abdominal cavity through four small skin incisions (0.5 – 1 cm, the incision above the belly button is a little longer: 2-3 cm) and the abdominal cavity is filled with gas (CO2) to create the necessary space and visibility for technical conduct of the operation. A camera is inserted into one skin incision (near the belly button); the surgeon sees its image on the monitor in the operating room. By manipulating special instruments the gallbladder is removed from the liver bed and the artery supplying the cystic duct and the gallbladder is closed by small metal clips.As a rule, wounds after laparoscopic surgery heal well and small scars that are usually barely visible remain. In case of the open method the wounds heal slower and the scar is bigger.
The main risks of laparoscopic cholecystectomy:
1. Injury of extrahepatic bile ducts (0.1—0.8%).
2. Injury of the neighbouring organs (duodenum and large intestine) (0.1—0.3%).
3. Bleeding from the gallbladder bed (liver) or hepatic porta (bleeding requiring switching to the open method up to 1%).
The operation lasts usually 25 – 90 minutes.
Usually, the patient is allowed to go home the next day after the surgery. Sutures are removed in 7 – 10 days. Most patients can return to work about a week after the surgery. In the immediate postoperative period it is reasonable to avoid high-fat foods and hearty meals.